|
Among patients with a MELD score < 25, the low-risk group also showed a better overall survival rate than the high-risk group with an independent association with decreased risk of all-cause mortality.Ĭonclusions: Patients with FI-lab < 0.5 showed a higher overall survival rate than those with FI-lab ≥ 0.5 in LDLT. The MELD score was originally developed as a valuable tool for assessing liver function and had been demonstrated to be associated with poor short-term. We were unable to demonstrate a difference in death-censored graft survival, rejection rate, or hospital stay. Furthermore, cox-regression revealed that FI-lab < 0.5 was independently associated with decreased risk of all-cause mortality (, 0.640, 95%, 0.454–0.902, p = 0.011). The 1-year, 3-year, and 5-year overall survival rates were 89%, 85%, and 75% for the low-risk group, while they were 78%, 76%, and 58% for the high-risk group. The low-risk group had a considerably greater overall survival rate than the high-risk group ( p < 0.001). 
Compared to the high-risk group (FI-lab ≥ 0.5), the Low-risk group was more likely to be male, to have hepatocellular carcinoma, and to have a low MELD score. Results: Among the total of 854 patients, those with FI-lab < 0.5 were 531. Given that the majority of LDLT patients have low model for end-stage liver disease (MELD) scores, we performed sensitivity analysis on patients with a MELD score < 25. Patients were separated into two groups according to FI-lab 0.5. 10 Given that average annual spending on an end-stage liver disease patient is reported to be US22 424, 10 prioritizing of the most critically ill patients for transplantation is increasingly important. Based on the current study demonstrating the superiority of MELD score at baseline, and previous studies, 16,17 we suggest that for future studies patients with alcoholic hepatitis be stratified at baseline into low mortality risk. 9 found that patients with MELD scores of 30 utilized 10 times more Medicare spending than those with MELD scores of 20. Those with less than 21 laboratory frailty index variables were excluded. The advantage of the MELD score is that the range is wide enough that finer stratification of risk is possible. The FI-lab score is calculated by adding all the scores and dividing them by the number of variables. Each result is granted a score of 1 if it falls outside the normal range. 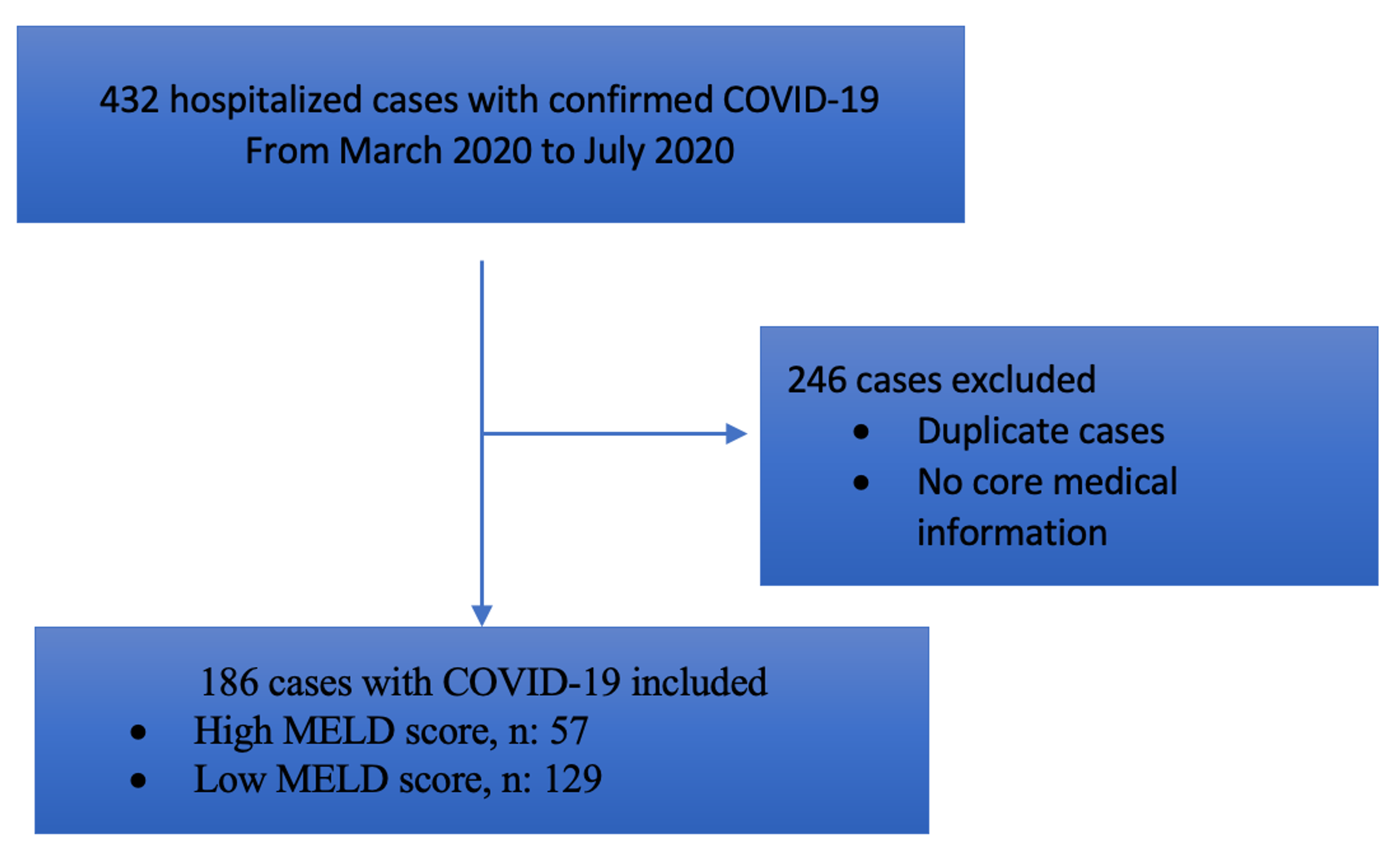
The FI-lab was made by taking 32 factors from standard blood test results and vital signs taken before surgery. Methods: Between 20, LDLT recipients from Severance Hospital were included. We aim to apply this index as a predictor for living-donor liver transplantation (LDLT). The laboratory frailty index (FI-lab) was found to be useful in the general population and valid among several frailty measurement scales. Abstract Background: Frailty is defined as the accumulation of deficits that increase vulnerability.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
